Spine
Read more about conditions we treat and surgical procedures we perform on the spine.

The Spine
The spine is a complex structure that supports the human skeleton. It consists of 7 cervical vertebrae(neck), 12 thoracic vertebrae (thorax), 5 lumber vertebrae (lower back) and the sacrum. The lumbosacral junction is the point where the spine connects to the pelvic bones.
The vertebrae surround and protect the spinal cord from which the spinal nerves emerge though the an opening between the vertebrae (intervertebral foramen). Between the vertebrae lie discs made of fibrocartilage and a gel like material within the centre.
Terms you may hear or read about:
Spondylolisthesis - refers to one vertebrae slipping out of alignment of the other.
Spondylolysis - commonly confused to the above term but refers to spine degeneration.
Compression or wedge fracture - a compressive injury of the spine where the front part is crushed down.
Burst fracture - a compressive injury of the spine where the vertebrae is fractured and spread in all directions.
Sciatica - pain that often starts at the back and radiates down the leg to the ankle and foot. Weakness and numbness are also features. Most of the time, sciatica is caused by a disc prolapse pressing on a nerve root. A typical disc prolapse at L4/5 tends to cause pressure on the L5 nerve root which manifests as pain going down to the outer aspect of the lower leg.
Disc prolapse - when a tear occurs in the outer fibrocartilage ring of the disc and allows the gel like material in the centre to herniate through.
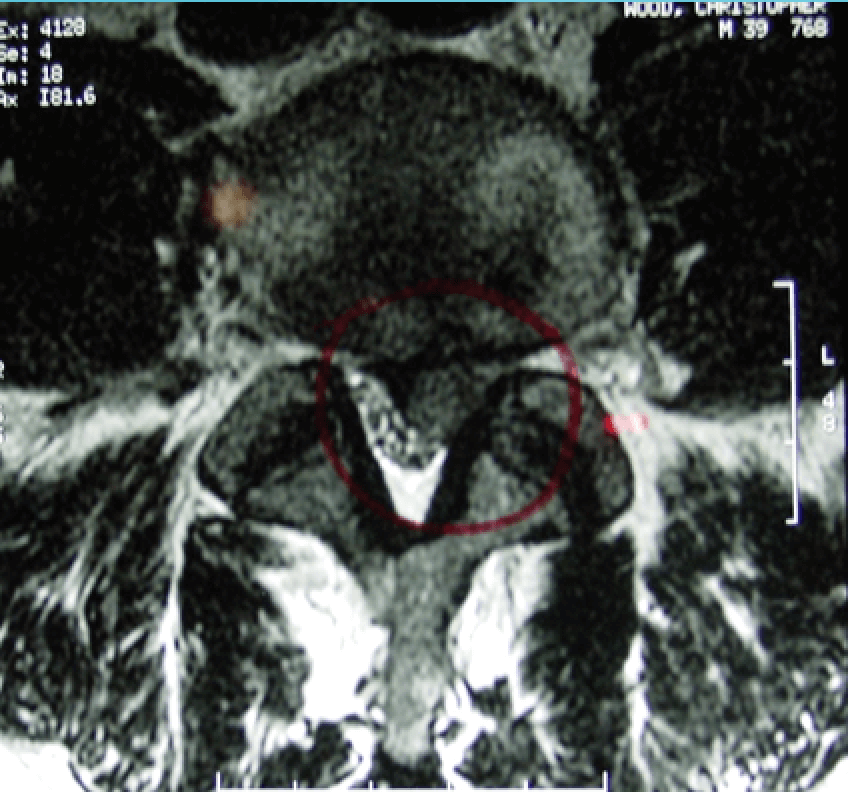
Scoliosis - refers to a curve in the spine. This can be congenital where the spine has developmental abnormalities like fused vertebra causing a curve or more commonly idiopathic (unknown cause) which occurs in adolescence. Significant curves may require bracing or surgical correction. Scoliosis can also be degenerative and occurs as the joints between the spine start to wear out.
Cauda equina syndrome - an emergency spinal condition where the lower nerve roots in the spine are compressed by a disc, tumour, trauma or narrowing of the spinal canal. This can manifest itself with severe back pain, loss of bladder and bowel control, leg weakness and numbness. This requires urgent investigation and treatment.
Spinal canal stenosis - stenosis describes narrowing of the spinal canal which can occur in the spine as a result of arthritis. This can lead to compression of the spinal cord which can cause pain and neurological disturbance such as weakness or numbness in the legs.
Degenerative Spinal Disease
As the body ages, wear and tear can affect all joints, including the spine. The discs start to lose their ability to cushion forces and the discs spaces narrow. This leads to more mechanical forces on the vertebrae and ligaments which lead to spurring and a change in position (sponylolisthesis).
Clinical presentation
Back pain is the most common presentation and this can be made worse by twisting or lifting objects. If a nerve is compressed by a disc or if there is spinal narrowing (stenosis), the pain can travel down the legs and be accompanied by numbness.
Management
The majority of back pain can be treated with non surgical means such as:
- analgesics like Panadol Osteo (paracetamol)
- anti-inflammatories like Celebrex (celecoxib) or Mobic (meloxicam)
- manipulation/massage
- back and core strengthening with physiotherapist/chiropractor or osteopath
- heat
Sometimes, cortisone injections to the joints in the back (facet joints) or nerves are appropriate.
Surgery
Surgery in the setting of a degenerative spine is most successful when there is some nerve or spinal cord compression. Surgery for back pain alone follows a less predictable course and is generally avoided.
If your surgeon deems it appropriate, he may opt to perform a laminectomy where the back part of the vertebrae is removed to give more room for the spinal cord. This most commonly occurs in the setting of spinal stenosis.
If there is compression of the nerve from a prolapsed disc then the disc can be removed via a microdiscectomy.
Spinal fusion is sometimes performed in combination with laminectomy surgery. This involves fusing the vertebrae together with metal implants like screws and rods as well as inserting a bone graft to complete the fusion.
Risks of spinal surgery
The results of spinal surgery in a carefully evaluated patient are good. The rate of complications is low but some of the risks include:
- nerve damage leading to altered sensation or leg weakness
- spinal cord damage (rare)
- deep vein thrombosis (DVT)
- infection
- dural leak (where the lining around the spinal cord is punctured and leaks spinal fluid. This can lead to headaches and may require further management
- bleeding
- post-operative spine instability
- failure of the spinal fusion (if performed)
- general anaesthetic complication
Procedures
Some of the procedures that Mr. De La Harpe performs include:
- Microdiscectomy
- Laminectomy
- Anterior Cervical Decompression and Fusion (ACDF)
- Lumber and Coccyx Injections
- Facet Joint Injections
- Lumbar Decompression and Fusion (Instrumented)
- Lumbar Decompression and Fusion (Non-Instrumented)
Microdiscectomy
The discs in the spine are made of an outer ring of fibrocartilage and an inner gel like material called the nucleus pulposis. The outer ring can get damaged by repetitive injury or an acute fall or lifting manoeuvre. This leads to herniation of the inner contents which can impinge or press on a nerve root. This causes pain radiating down the limb.
Management
Disc prolapses or herniations can resolve by themselves and the symptoms can be controlled by:
- strong analgesics like oxycodone
- anti-inflammatories
- Valium (diazepam) for back spasm
- limited bed rest
Epidural injections or nerve root injections can also be helpful.
Surgery
If the pain is not well controlled or if the symptoms do not appear to settle with time then surgery may be appropriate.
Removal of the herniated disc material can be performed via a standard open incision or via a microdiscectomy. The latter is a minimally invasive approach allowing the surgery to be performed though a small incision and often uses an operating microscope to visualise the nerve roots to allow the disc to be removed safely.
The minimally invasive approach allows a quicker recovery with less pain.
Laminectomy
When the spinal canal or the bone around the exiting nerves compresses the nerve, this can cause pain that radiates down a limb.
If conservative measures have failed, a laminectomy can be performed which is when the back portion of the vertebra (the lamina) are removed to allow more room for the cord and nerves.
Spinal Fusion
In appropriate cases where there is significant spine degeneration with instability and nerve compression, a spinal fusion can be performed. Treatment usually involves decompression of the spinal canal or nerve roots followed by stabilisation of the spine. This can be an instrumented fusion where the spine is fused with rods and screws with bone graft. Fusion can also be non-instrumented with only bone graft used in selected cases.
LOCATIONS
For all appointments and enquiries contact us on:
9:00am - 4:00pm Monday - Friday
Prof Martin Richardson
Mr David de la Harpe

