Hip
Read more about conditions we treat and surgical procedures we perform on the hip.

Total Hip Replacement
Osteoarthritis or “wear and tear" of the hip is a common problem. There are also other forms of arthritis like rheumatoid arthritis which can affect the hip. Some childhood conditions like DDH (developmental dysplasia of the hip) or Perthe’s Disease may lead to osteoarthritis at a younger age.
The pain from a degenerative hip typically manifests itself with groin and buttock discomfort but can also present as thigh or knee pain. The symptoms can limit activities of daily living due to the pain and stiffness.
Initial Management
Initial measures include activity modification such as avoiding impact activities like running, analgesics like Panadol Osteo (paracetamol) and anti-inflammatories like Nurofen (ibuprofen) or Mobic (meloxicam).
Procedure information
At some stage, the symptoms can worsen to a level where the pain is not well controlled. It is at this point that a total hip replacement is offered to the patient. This involves replacing the hip socket (or cup) with a metal one (usually titanium) lined by a highly cross-linked polyethylene or ceramic. The femoral head (or ball) is replaced by a metal stem and head.
Total hip replacements have been around for over 30 years and the current designs have shown excellent results in terms of function and longevity.
Excellent results are achieved with all surgical approaches to the hip. More information on anterior hip replacement can be found above.
Joint replacements are common operations but are still considered a major surgery with great benefits but also risks of complications. In assessing patients for a joint replacement, the aim is to ensure that the operation is appropriate for the patient’s stage of disease and that any risks are minimised by optimising any other medical conditions. The risks and benefits of surgery will be discussed.
Most complications are temporary setbacks. The results of hip replacements are generally considered to be excellent and the strong likelihood is that you will undergo the operation without any problems.
Some complications of total hip replacements include:
- blood clots
- postoperative infection
- loosening of the prosthesis from bone
- dislocation of the hip - there is an increased risk within the first 6 weeks after surgery. This complication can be avoided by observance of the post-operative instruction
- fracture
- residual pain and stiffness can occur
- leg length discrepancy
- damage to nerves or blood vessels
- allergy to the prosthesis (rare)
- anaesthetic issues
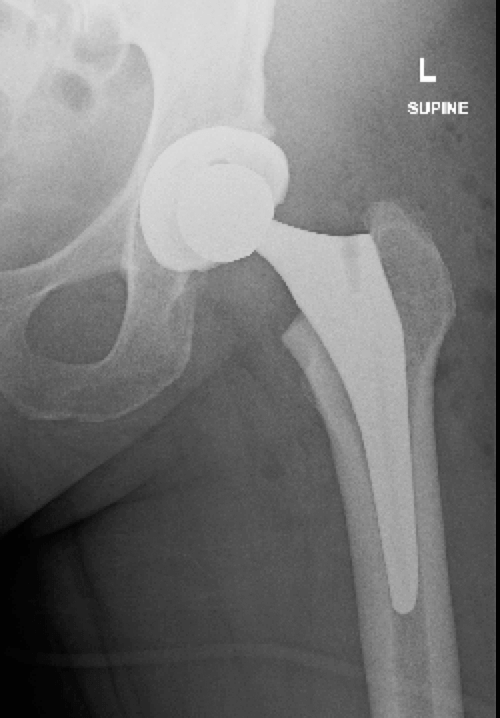

What to expect
How long will I be in hospital?
This procedure is a moderately large orthopaedic procedure and usually requires 4-5 days in hospital and sometimes requires a further in-patient period of rehabilitation.
When can I walk on the leg?
You can usually fully weight bear within 24 to 48 hours of surgery with the assistance of physiotherapy and walking aids.
What are the risks of surgery?
This operation, as with any others, requires an anaesthetic which in a fit, healthy young person is relatively straightforward. Specific anaesthetic risks will be discussed with your anaesthetist.
Risk of deep infection following this procedure is about one in 200. This is minimized by antibiotics given in your drip for 24 to 48 hours following your surgery.
A blood clot in the veins of the calf (deep venous thrombosis) is a potential risk but a blood thinning injection (heparin) will be given to you at the time of your operation to thin the blood enough to minimise this risk. If a blood clot should form, break off and go to the lungs, it can be serious and you must report any shortness of breath, coughing up of blood or severe chest pain, which may indicate a pulmonary embolus.
What happens if I get an infection?
This is a major problem and may require washing out of the hip with further surgical procedures.
Will there be anybody else involved in my care?
Your surgeon has a strong team involved in managing your operation including a fully qualified consultant anaesthetist, surgical assistant and physician to help manage associated medical issues.
When can I drive?
Following a hip replacement, a 4-6 week period not driving a car is recommended. The key to the decision on driving is whether you can safely stop in an emergency situation. You can be guided by sitting in a stationary vehicle in your driveway, imagining an emergency situation and attempting to make the appropriate avoidance procedures. If this is uncomfortable, you will know it is not safe to begin driving at this stage.
How long will it take to recover from total hip replacement surgery?
It will take 3 to 6 months to fully recover from this operation.
Revision Total Hip Replacement
In some circumstances, a total hip replacement may have to be removed and revised.
Loosening
Hip replacements are mechanical devices with bearing surfaces that can wear out. This can result in wear particles that can cause the cup (the acetabular component) or stem (femoral component) to loosen. A consequence of this can be bone loss and soft tissue damage. Fortunately, the modern hip replacement is proving to be very durable and early revisions for loosening are uncommon.
It is important to have your hip replacement checked if it is over a decade old and if you notice any change in function or develop pain.
If these hip replacements start to loosen then a revision hip replacement can be contemplated.
Infection
Another reason for revision hip replacement is infection. Unfortunately, one of the complications of a joint replacement is infection. This can either occur at the time of implantation or it can occur from bacteria lodging in the joint from the bloodstream. An infection in a joint replacement is serious and can cause the joint to fail or make the patient unwell.
If there is suspicion of infection, an urgent assessment is warranted. The hip may need to be investigated with blood tests, imaging and aspirations before definitive treatment.
An established infection may require the old components to be removed with placement of a temporary hip made of antibiotic cement. This is replaced with the definitive revision total hip replacement after a period of antibiotics.
Dislocation
Hip replacements can become unstable with the head dislocating from the joint. Although they function very well, the design constraints of artificial joint replacements mean that they are unable to completely mimic the natural anatomy of the hip.
Instability can be due to several factors, including lack of patient compliance with early restrictions, component positioning issues or soft tissue tension problems.
A recurrent problem can lead to revision of the hip replacement.
Pain
A revision hip replacement is a bigger operation than a primary hip replacement. While the components may start to loosen, they are often still fixed to parts of the bone and removing them can be time consuming and risks removal of more bone. The operations are more complex, take more time and may involve a greater risk of blood loss, infection, fracture and damage to nerves and blood vessels.
It is important to discuss the case with your surgeon.
For all appointments and enquiries contact us on:
9:00am - 4:00pm Monday - Friday
